Gentle Yoga for Fibromyalgia
1. Understanding Fibromyalgia and Movement
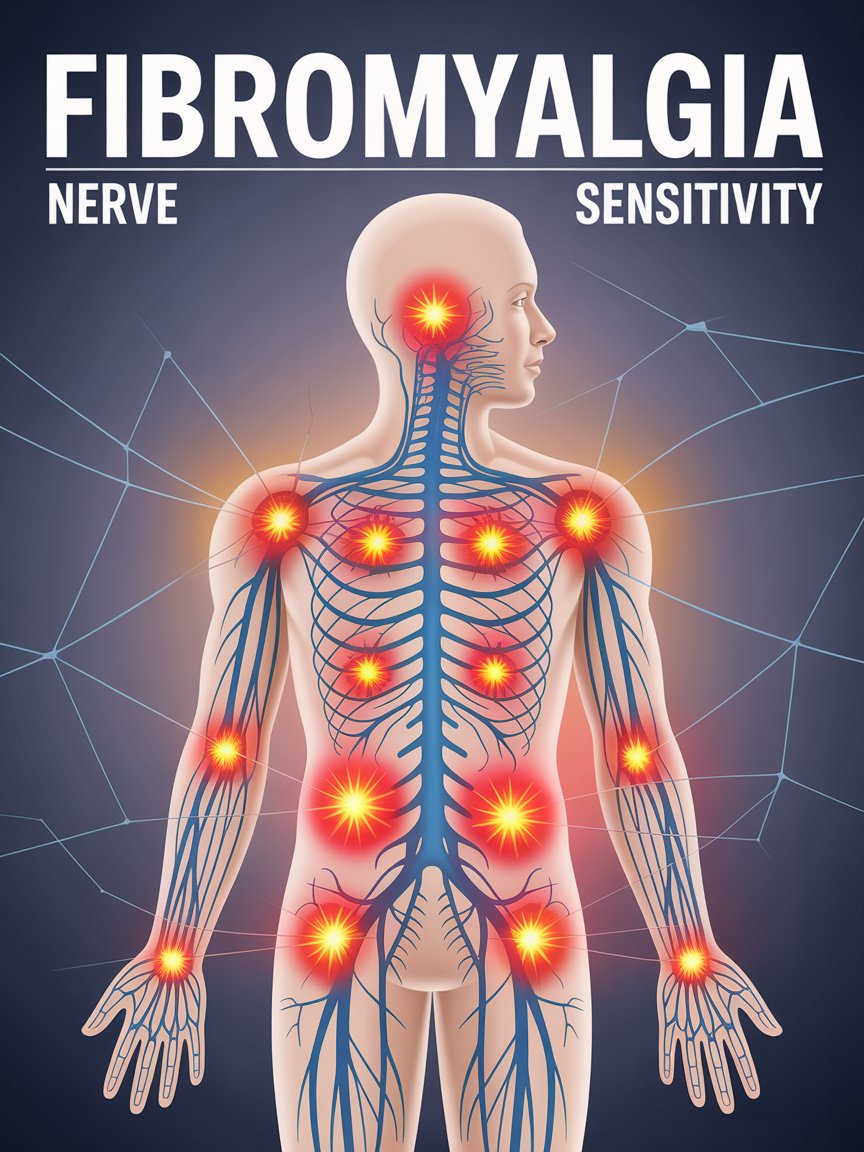
Fibromyalgia is a condition that causes widespread pain, fatigue, and muscle stiffness. Many people worry that physical activity might worsen their symptoms. However, gentle movement such as yoga can actually help improve flexibility and reduce discomfort.
2. What Is Gentle Yoga?
Gentle yoga focuses on slow movements, controlled breathing, and simple stretches. Unlike intense workout styles, it emphasizes relaxation and body awareness. This makes it especially suitable for people managing chronic pain conditions.
3. Benefits of Yoga for Fibromyalgia
Yoga can help improve muscle flexibility and joint mobility. It may also reduce stress and support better sleep. Over time, regular practice can contribute to improved overall well-being.
4. Reducing Muscle Stiffness
Stiff muscles are a common symptom of fibromyalgia. Gentle stretching through yoga helps loosen tight muscles and improve circulation. This may reduce the feeling of tension throughout the body.
5. Supporting the Nervous System
Fibromyalgia is often linked to increased sensitivity in the nervous system. Yoga’s combination of movement and breathing encourages relaxation. This may calm the nervous system and reduce pain sensitivity.
6. Improving Balance and Stability
Slow yoga poses help strengthen muscles that support balance. This is important for preventing falls and improving physical confidence. Even simple poses can make a difference over time.
7. The Importance of Slow Progress
People with fibromyalgia should approach yoga gradually. Starting with short sessions and basic poses prevents overexertion. Listening to the body is essential for avoiding flare-ups.
8. Breathing Techniques in Yoga
Deep breathing is a central part of yoga practice. Controlled breathing increases oxygen flow and helps relax the body. It can also reduce stress and tension that worsen fibromyalgia symptoms.
9. Seated Yoga Poses
Seated yoga poses are often comfortable for beginners. They allow gentle stretching of the back, shoulders, and neck. These poses can be practiced on a chair or yoga mat.
10. Gentle Stretching Poses
Simple poses such as child’s pose, cat-cow stretch, and gentle spinal twists are commonly recommended. These movements improve flexibility without placing too much pressure on the body. They are especially helpful for relieving stiffness.
11. Using Props for Support
Yoga props such as cushions, blankets, and blocks provide extra support. They help maintain proper posture and reduce strain. Using props allows individuals to practice safely and comfortably.
12. Creating a Relaxing Environment
Practicing yoga in a quiet and comfortable space can enhance relaxation. Soft lighting and calming music may make the experience more enjoyable. A peaceful environment supports both physical and mental benefits.
13. Combining Yoga With Other Treatments
Yoga works best when combined with other fibromyalgia management strategies. Balanced nutrition, proper sleep, and medical care all contribute to overall health. Together, these approaches support symptom relief.
14. Staying Consistent With Practice
Consistency is key when practicing gentle yoga. Even short sessions a few times per week can provide benefits. Over time, regular practice may improve strength, flexibility, and stress levels.
15. Building a Sustainable Routine
Gentle yoga offers a supportive way to stay active while living with fibromyalgia. By moving slowly and respecting personal limits, individuals can gain both physical and emotional benefits. With patience and consistency, yoga can become a valuable part of daily self-care.